Acute Flaccid Monoplegia After an Asthmatic Attack
Keywords:
Hopkins syndrome, Monoplegia, Acute asthmatic attack, Asthmatic amyotrophyAbstract
Background: Hopkins syndrome is a polio-like paralytic illness following a few days after asthmatic attack. Although very rare, the disease has devastating clinical outcomes.
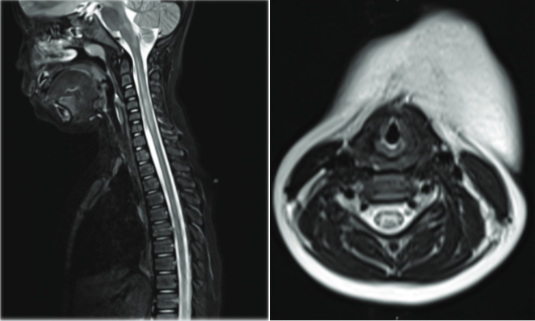
Case Report: The patient was a 4-year-old girl presenting with acute monoplegia of her right arm six days after an event of acute asthmatic attack. Magnetic resonance imaging revealed increased T2 signal intensity within the cord from C1 to C6-7 levels, mainly at anterior horns. The patient did not gain motor power improvement after two years of treatment and follow up.
Conclusions: We report a rare case of Hopkins syndrome presented with acute flaccid monoplegia and magnetic resonance imaging pathology. This is the first case report in Southeast Asia
Downloads
References
Gateau KL, David H, Lowe CG. Hopkins Syndrome: Post Flaccid Paralysis After an Asthma Exacerbation. Pediatr Emerg Care. 2019;35(10):190-191.
Kumar P, Kumar P, Ry K. Monocrural flaccid paralysis following asthmatic attack (post asthmatic amyotrophy) - case report & minireview. Clin Neurol Neurosurg. 2014;123:1-3.
Hayashi F, Hayashi S, Matsuse D, Yamasaki R, Yonekura K, Kira JI. Hopkins syndrome following the first episode of bronchial asthma associated with enterovirus D68: a case report. BMC Neurol. 2018;18(1):71.
Hopkins IJ. A new syndrome: poliomyelitislike illness associated with acute asthma in childhood. Aust Paediatr J. 1974;10(5):273-276.
Manson JI, Thong YH. Immunological abnormalities in the syndrome of poliomyelitis like illness associated with acute bronchial asthma (Hopkin’s syndrome). Arch Dis Child. 1980;55(1):26-32.
Cohen HA, Ashkenasi A, Ring H, et al. Poliomyelitis-like syndrome following asthmatic attack (Hopkins’ syndrome)--recovery associated with i.v. gamma globulin treatment. Infection. 1998;26(4):247-249.
Arita J, Nakae Y, Matsushima H, Maekawa K. Hopkins syndrome: T2-weighted high intensity of anterior horn on spinal MR imaging. Pediatr Neurol. 1995;13(3):263-265.
Horiuchi I, Yamasaki K, Osoegawa M, et al. Acute myelitis after asthma attacks with onset after puberty. J Neurol Neurosurg Psychiatry. 2000;68(5):665-668.
Cantarin-Extremera V, Gonzalez-GutierrezSolana L, Ramirez-Orellana M, Lopez-Marin L, Duat-Rodriguez A, Ruiz-Falco-Rojas ML.
Immune-mediated mechanisms in the pathogenesis of Hopkins syndrome. Pediatr Neurol. 2012;47(5):373-374.
Pavone P, Longo MR, Scalia F, Polosa R, Kira J, Falsaperla R. Recurrent Hopkin’s syndrome: a case report and review of the literature. J Neurol Sci. 2010;297(1-2):89-91.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2022 Asian Medical Journal and Alternative Medicine

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.


